Course Authors
Sheryl Merkin, M.S., F.N.P., C.D.E., Sharon Movsas, M.S., R.D., C.D.E. and Joel Zonszein, M.D., C.D.E.
Release Date: 06/11/2019
Upon completion of this Cyberounds®, you should be able to:
State the recommendations for glucose monitoring and diet in individuals receiving intensive insulin therapy;
Explain the basic principles of insulin replacement hormone utilizing basal/bolus regimens;
Identify the new insulins and new insulin delivery systems.
Case Report The patient is a 51-year-old, white male with new-onset diabetes. He has a strong family history of diabetes. His BMI is 17 kg/m2, he is normotensive and has had hypercholesterolemia treated with atorvastatin 10 mg daily; his triglycerides and HDL-cholesterol were normal. The patient did not have evidence of any chronic diabetic complications. Laboratory results showed an initial HbA1c of 11%, a low C-peptide (0.7 ng/ml) and high antibodies to glutamic acid dehydrogenase (anti-GAD) (49.5 U/ml). The diagnosis of Latent Autoimmune Diabetes of the Adult (LADA) was established. The patient was treated initially with a regimen consisting of fixed doses of Novolog mix 70/30® pen syringe (recombinant DNA human insulin with 70% protamine aspart suspension and 30% soluble aspart insulin) before breakfast and before dinner. With this regimen, he developed several hypoglycemic episodes. Because of inadequate counseling and education by the initial physician, the patient decided to change endocrinologists. He was seen by a second endocrinologist who believed in the team approach and who worked with a nurse and nutritionist who were both Certified Diabetes Educators (CDE). After evaluation and education, the insulin regimen was changed to Lantus® glargine given in the morning and the patient was instructed to self-adjust the dose according to his pre-meal blood sugars. On this regimen, his blood glucose values improved significantly. He felt well, resumed his usual work hours and sports activities without further episodes of hypoglycemia. He came for a follow-up visit to review his insulin regimen. |
Metformin, an oral agent that decreases hepatic glucose production, has no indication in the treatment of Type 1 diabetes.
Nateglinide, an oral agent that causes insulin secretion, has no indication in the treatment of Type 1 diabetes.
Pioglitazone, an oral agent that causes insulin sensitivity, has no clear role or indication in the management of individuals with Type 1 diabetes.
The patient has improved insulin secretion and better glycemic control as a result of insulin therapy and resolution of glucose toxicity. This window of improvement in glycemic control is also known as the "honeymoon period of the disease," tends to vary in time, but is often associated with mild hyperglycemia that can cause chronic complications(1)(2)(3)(4)(9) and less islet β-cell function later in the course of the disease.(6) Delaying intensive insulin treatment, therefore, will be conterproductive in these patients. This strategy needs to be explained as part of the necessary education for individuals with Type 1 diabetes, i.e., intensive insulin therapy is recommended.
After the Diabetes Control and Complications Trial (DCCT) findings showed that improved glycemic control with intensive insulin therapy in patients with Type 1 diabetes mellitus led to significant reductions in retinopathy, nephropathy, neuropathy particularly and microvascular complications to a lesser extent,(1)(2) achieving glycemic control as close to normal (A1C 6-7%) without meaningful hypoglycemia has become the standard of care.
Insulin Overview
Insulin administration is meant to mimic the body's natural insulin production to achieve certain glycated hemoglobin (HbA1C) and blood glucose targets. Typical regimens have usually been done in a basal/bolus method with long or intermediate insulins given as basal dosing and pre-meal regular or short-acting insulin as the boluses. These insulin formulations can be injected separately or mixed in the same syringe. Rapid-acting insulins are available as analogues which include insulin lispro, insulin aspart, insulin glulisine and a non-injectable rapid acting inhaled insulin, (Afrezza®), though use of the latter has been limited. These insulins better mimic naturally-secreted meal insulin bursts when compared to regular insulin. Long-acting insulins are also available as analogues. These include glargine, detemir and degludec which have quickly replaced the intermediate-acting insulins such as lente and NPH, and the long-acting insulin, ultralente.(10) The long-acting insulin analogues are more predictable with less variability in glycemic changes. Table 1 includes a complete list of all types by category.
Table 1. New and Commonly Used Insulins: Basal and Bolus.
| Peak | Hours | ||
|---|---|---|---|
| Rapid Acting | |||
| Lispro (Humalog, Admelog) | 1-2 | 2-6 | |
| Aspart (Novolog) | 0.5-1 | 2-6 | |
| Glulisine (Apidra) | 1-2 | 1-4 | |
| Insulin human [inhaled] (Afrezza) | 0.25-0.5 | 2-3 | |
| Short-Acting | |||
| Regular (Humulin R, Novolin R) | 2-5 | 3-6 | |
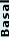 |
Intermediate-Acting | ||
| NPH | 6-12 | 10-24 | |
| Long-Acting | |||
| Glargine (Basaglar, Lantus, Toujeo) | none | 20-24 | |
| Detemir (Levemir) | none | 12-24 | |
| Degludec (Tresiba) | none | ~42 | |
Current available types of insulins with corresponding peak onset and duration listed in hours. Brand names listed in parentheses. Modalities other than intermittent subcutaneous injection in brackets.

Conventional insulin therapy regimens use a single daily injection, or two injections per day (regular and NPH insulin, mixed together in the same syringe, given in fixed amounts before breakfast and dinner). This is now replaced with insulin regimens providing a basal bolus approach. The stable basal insulin is given as one to two daily injections of intermediate- or long-acting insulin, or via continuous subcutaneous insulin infusion (insulin pump). Bolus insulin — regular insulin, rapid-acting insulin analogues or the rapid-action inhaled insulin — is given in addition to the basal insulin before each meal. It is worth mentioning that available inhaled insulin formulations have fallen out of favor due to problems with absorption, increased hypoglycemia and increased respiratory adverse effects.(36) The choice of regimen and type of insulin is individualized and depends on each patient's lifestyle and preference.(12) For optimal insulin regimens, understanding insulin pharmacokinetics is critical, as the duration of action is affected by such factors as the type of insulin preparation, insulin dose, injection technique and site of injection.(13)
Patient education about insulin addresses a few basic issues — unused vials should be refrigerated and both extreme temperatures and excess agitation avoided — to preserve its potency. When clumping, frosting or precipitation are noticed, the insulin should be replaced. An extra bottle of each type of insulin used should always be available.
Conventional insulin administration involves injection with syringes that are now available as 0.3 cc (up to 30 units), 0.5 cc (up to 50 units), and 1 cc (up to 100 units) with smaller (30 and 31 gauge) needles of several lengths. Prescriptions should specify the type of syringe and needle. When pen syringes are used instead of the classical syringes, prescriptions for the pen syringe, as well as the pen needles, also need to be specific. Insulin syringes and pens, needles and lancets should be disposed properly either through needle disposal programs or placed in a puncture-resistant container; local trash authorities should be contacted for proper disposal and to assure that these containers will not be recycled.

Figure 1. Insulin Pens.
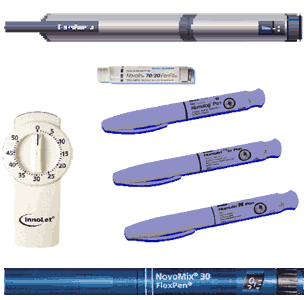

Basal Insulins: Intermediate and Long-Acting
Exogenous basal insulin is provided continuously throughout the day with the goal of normalizing non-meal related blood sugars. Although it is meant to resemble the sustained non-meal related endogenous insulin, a true physiologic replication is extremely difficult. Also, insulin is administered peripherally and not via the portal system that is the case with endogenous insulin that is constantly changing in response to the provision of fuels and the regulation of many other hormones. Thus exogenous insulin with fixed absorption rates and duration of action cannot replicate the intricate endogenous insulin secretion.
Until recently, NPH has been the classic basal insulin, used widely in DCCT.(2) In Type 1 diabetes, NPH insulin should be given as two injections — in the morning and at bedtime. The bedtime dose attempts to take advantage of its peak — the maximum insulin oncentration/effect that occurs six to seven hours later — to meet the increased insulin demands that take place in the morning (dawn phenomenon). When given before dinner NPH may cause hypoglycemia as it typically peaks around 3:00AM, the same time of the physiologic glucose nadir. In practice, however, NPH peaks are difficult to predict because of high intrapatient and interpatient variability. Thus, the long-acting insulin analogues (glargine, degludec and detemir) provide more steady basal replacement, resulting in less hypoglycemia and less hyperglycemia. Though they offer better control, they still do not replicate physiologic secretion of basal endogenous insulin production. Another advantage of the long-acting insulin analogues is improved absorption leading to less intra-patient variability, allowing for more predictability. (14)
Insulin glargine, introduced in 2001, was the first insulin analogue with a prolonged duration of action to become available. (15) Insulin glargine differs from human insulin in that the amino acid asparagine at position A21 is replaced by glycine and two arginines are added to the C-terminus of the β-chain. These amino acid changes reduce the aqueous solubility of insulin glargine at physiologic pH, stabilizing the hexamers and delaying its dissociation into monomers. It is released gradually from the injection site with a slow absorption which results in a relatively constant basal insulin supply. Glargine is formulated as a clear acidic solution and because of its low pH cannot be mixed with other insulins.(16) Therefore, a basal/bolus regimen using glargine requires four injections a day compared to a basal/bolus regimen using NPH which requires three injections a day. Glargine comes in U-100 and U-300 formulations. U-300 glargine is newer and delivers the same number of units in a smaller volume. The smaller insulin depot reduces the surface area leading to a slower release of insulin overtime, which results in a longer duration and a more predictable pharmacologic profile. (14)
While NPH insulin has a peak action at six to seven hours after injection, with detectable serum insulin concentration levels after 17 hours, insulin glargine only has a small peak at four hours and remains active at 24 hours. Studies comparing NPH twice-daily plus two pre-meal boluses at breakfast and dinner to glargine once-daily plus three pre-meal boluses have shown that the glargine regimen has fewer hypoglycemic episodes, particularly nocturnal hypoglycemia, lower fasting blood glucose concentrations and produces the same or slightly improved A1C values.(17)(18) While many patients achieve stable basal serum insulin concentrations with a single daily injection of glargine, given in the morning or evening (it is approved to be given at any time of the day), some patients with Type 1 diabetes may need twice-daily insulin injections.
Insulin detemir, approved by the FDA in June 2005, was the second long-acting insulin analogue.(19) The prolonged action of this insulin is attributable to the addition of a fatty acid side chain that allows a constant albumin binding and unbinding which results in a steady insulin serum concentration and less variability of blood glucose concentration. The duration of action is dose-dependent but appears to be shorter than that of insulin glargine. Insulin detemir, brand name Levemir®, has been approved by the FDA to be used once or twice daily in patients with Type 2 or Type 1 diabetes. Glycemic control appears to be superior with detemir in trials comparing twice daily insulin detemir and NPH.(20) Additionallly, insulin detemir is associated with less nocturnal hypoglycemia, better fasting blood sugars and less weight gain.(21)(22)(23)
Insulin degludec is an ultra-long acting insulin analogue approved by the FDA in 2015. It has a deletion of the threonine amino acid residue at B30 and the addition of a fatty acid to lysine at B29, and is formulated with zinc.(14) The drug self-aggregates and forms stable multi-hexamers. Diffusion of zinc from these results in a slow absorption of the insulin, leading to stable and continuous delivery.(24) Analyses have shown that the effect is evenly distributed across the entire half-life of the drug (25 hours), with decreased intra-patient, day-to-day variability of its glucose-lowering properties.(24) Studies from the BEGIN clinical trial program investigating degludec, found significant reductions in mean daily basal, bolus, and total insulin required with degludec compared to glargine- with the implication that if switching a patient from glargine to degludec doses may need to be reduced. (24) No significant differences in rates of overall hypoglycemic episodes were found in the BEGIN trials focusing on degludec vs glargine in Type 1 diabetics.(24) Given its longer half-life and stable delivery, degludec also allows for flexibility of timing once daily doses to adjust to different lifestyles without large fluctuations of insulin in circulation that may be seen in other basal insulins.
Although the patient's glycemic control improved significantly and he was doing fine with basal insulin only, evidence based medicine supports a more aggressive approach in order to reduce the risk of diabetic retinopathy, nephropathy, neuropathy(2)(3)(6)(7)(8) and macrovascular complications.(1) Intensive therapy markedly reduces the risk of progressive retinopathy and is more effective when introduced during the first five years.(2) The mechanisms by which early intensive insulin management prevents long-term complications known as the "metabolic memory" are unclear;(9) any elevation in glycemia, even in the subdiabetic range, can increase the risk for cardiovascular disease.(11) Thus, implementation of intensive insulin therapy as early as possible and maintenance of good glycemic control as long as possible result in a short- and long-term reduction of complications. Also early intensive insulin treatment results in better metabolic control short and long term, probably by preserving beta cell function.(13)
Changing from glargine to detemir at bedtime will not improve glycemic control. Detemir works for 12 hours, thus two injections are often required. The advantages of switching to detemir are less hypoglycemia, less weight gain and improvement in fasting blood glucose, none of which was an issue at this time in this case.
Changing from glargine to two injections of detemir will not improve glycemic control. While advantages of switching to Levemir are less hypoglycemia, less weight gain and improvement in fasting blood glucose, none of which was an issue at this time in this case.
Glargine, a basal insulin, cannot prevent postprandial glycemic surges in insulinopenic individuals. Sooner or later, the patient will need to add pre-meal bolus injections. There is plenty of evidence that earlier and more aggressive treatment will result in fewer complications and better glycemic control.(1)(2)(3)(6)(7)(8)(9)(11)
This patient already has an effective basal regimen. Switching to two injections of NPH will cause more glucose variability, because of the NPH peaks, so that a bolus regimen will still be necessary.
Case Report, Continued During a follow-up visit with the nurse, blood glucose records showed significant improvement but, based on his diagnosis of Type 1 diabetes, a more intensive regimen was indicated. After education was provided on the intensified regimen, including relevant changes in glucose testing, insulin administration and record-keeping, a basal-bolus regimen was prescribed. The patient was resistant to intensifying the regimen, as it meant more injections, and requested information about Exubera®, the inhaled insulin. We advised the patient against an inhaled insulin because of its known adverse pulmonary effects (see above) and instead suggested he start a basal bolus regimen with a fixed dose of rapid-acting Apidra® (insulin glulisine), three units before each meal, which he agreed to do. The basal insulin was reduced from 12 to 8 units daily to avoid hypoglycemia because, typically, basal insulin is about 40-60% of the total daily dose. He was also referred to a dietitian for carbohydrate counting, a skill needed for self-adjustment of pre-meal insulin boluses according to the meal. |
A more intensive insulin regimen is necessary not only to avoid chronic diabetic complications but also for preservation of beta cell function and easier management.(13) Since the patient has adequate basal insulin, bolus insulin will improve postprandial glycemias. Bolus insulin doses change constantly and need to be calculated by the patient according to the blood sugar level (correction factor), carbohydrate to insulin ratio (CIR) related to insulin sensitivity and carbohydrate content of each meal. Since education for self-insulin adjustments takes some time, he was initially prescribed a fixed dose.
Bolus Insulins: Rapid-acting Analogs, Regular and Inhaled
In addition to regular insulins, there are three rapid-acting injectable insulins and one inhaled insulin that can be used for pre-meal boluses. Rapid-acting insulin is designed to have a faster onset and shorter duration than regular insulin. Modifications made to the insulin molecule, by substituting an amino acid(s) in the β-insulin chain, permit faster absorption, quicker peak action and shorter duration (see Table 1).
Compared to regular insulin, rapid-acting insulins allow easier timing with meals, achieve better reductions in postprandial hyperglycemia and provoke fewer instances of hypoglycemia.(25) But they also may result in hypoinsulinemia and hyperglycemia five to seven hours after injection due to their shorter duration of action.(26) When this occurs, it is necessary to increase the dose of the intermediate or long-acting insulin.
Rapid-acting insulins are more convenient for patients using intensive insulin therapy, as they correct hyperglycemia more rapidly than regular insulin. These effects appear to be equally effective in the three analogues.(27)(28)(29) Results from clinical trials show only small differences in the reduction of A1C between the analogues and regular insulin.(30) Rapid-acting insulins cost more, and the possibility of teratogenicity and long-term safety are unknown. Ideally, rapid acting insulins are given around 10-20 minutes before a meal, since giving it before (as opposed to during) has been shown to reduce post-prandial glucose spikes more. (14)
Insulin lispro was the first commercially available analogue. Lispro is identical to human insulin except for a reversal of the B28th and B29th amino acid residues (proline and lispro, respectively), permitting it to act similarly to monomeric human insulin. Lispro has the pharmacokinetic profile of the rapid acting insulins and thus better mimics the normal prandial insulin surge in response to carbohydrate ingestion.(31)
Insulin aspart was the second rapid-acting analogue, engineered through replacement of the proline residue at position 28 of the β-chain with aspartic acid. The replacement decreases self-association of insulin aspart monomers, resulting in a pharmacokinetic profile similar to lispro's, and it is, thus, well suited for use as meal insulin.
Insulin glulisine was FDA approved in April 2004.(32) This rapid-acting insulin analog differs from human insulin by the replacement of the amino acid asparagine with lysine at position 3 and lysine with glutamic acid at position 29 of the β-chain. Compared with regular insulin, and similar to other rapid analogues, glulisine has a more rapid onset of action and a shorter duration of action.(33)
Inhaled insulins present an attractive option for bolus insulin in patients with diabetes. They were first introduced into the U.S. market in 2006 with Exubera, but Exubera was discontinued the next year after poor sales.(34) Afrezza (human insulin) was approved by the FDA in 2014.(35) Inhaled insulin may be used in diabetic adults who do not smoke or have any lung disease. Their use has fallen out of favor due to numerous concerns with administration, delivery, hypoglycemia and adverse pulmonary effects.(36)

Figure 2. Insulin Inhaled Device (Afrezza)

The Afrezza inhaler device on the left with its different insulin cartridges on the right with their corresponding units of insulin. (37)

Fixed combinations insulins are commercially prepared mixtures where the basal and bolus insulins are divided with the intention (unsuccessful) of replicating physiological insulin production.(14) However, they do serve a purpose, especially initially in patients who require a simpler and more convenient method of physiologic insulin replacement, but glycemic control is often hard to achieve because they limit optimal individualized basal-bolus needs.(5) Novolog 70/30, for example, is a fixed combination (70% of protamin aspart suspension and 30% soluble aspart insulin; all recombinant DNA human insulin) that is given twice daily before breakfast and dinner at a prescribed dose without self-adjustment. The protamine component of the aspart and lispro premixed insulins functions like NPH.(15) While simpler to implement, this type of regimen is associated with long-term weight gain and hypoglycemia, both of which often lead to compromised adherence. As the name suggests, "fixed combinations" limit individualization and flexibility; raising basal insulin requires raising the bolus insulin and vice versa. Insulin dosage adjustments based on basal needs can impose a dietary modification to offset the increase in bolus insulin. Hence, patient education on consistency of meal timing and carbohydrate content is indicated.
Insulin preparations with a predetermined proportion of intermediate-acting insulin mixed with short- or rapid-acting insulin (e.g., 70 percent NPH/30 percent regular, 50 percent NPH/50 percent regular and 75 percent NPL (protaminized insulin lispro)/25 percent insulin lispro) are also available and are shown in Table 2.

Table 2. Fixed-Mixed Insulins.
Humulin (NPH/regular) 70/30 and 50/50 (NPH/regular) Humalog 75/25 (Prot-lispro/free lispro) Novolin 70/30 (NPH/regular) Novomix 70/30 (Prot-aspart/free aspart) |
The percentage of rapid or very rapid insulin is shown as the denominator.

Pramlintide Acetate
Pramlintide acetate (Symlin®) is a synthetic analogue of human amylin, an islet amyloid polypetide hormone secreted by the pancreatic beta cells simultaneously with insulin in response to nutrient stimuli, that slows gastric emptying, reduces postprandial rises in blood glucose concentrations and improves A1C values. The FDA has approved pramlintide for use in patients with Type 1 and Type 2 diabetes. This non-insulin, injectable amylin analogue is administered by mealtime subcutaneous injection before meals, cannot be mixed with insulin in the same syringe and in patients with T1DM is not a replacement for but rather an addition to pre-meal insulin bolus injections.
Pramlintide regulates post-meal blood glucose levels by slowing gastric emptying and suppressing the abnormal postprandial rise of glucagon in patients with diabetes.(43) Thus, hepatic glucose production is better regulated. The effects on hepatic glucose production and increased insulin production are glucose-dependent and are overridden as serum glucose levels fall. In individuals with Type 1 diabetes, 30 to 60 mcg of pramlintide administered subcutaneously with meals resulted in sustained reductions in A1C with modest reductions in body weight.(44)(45) Hypoglycemia and nausea are the most commonly reported side effects. Nausea generally dissipates with time and can be minimized by slow upward dose titration.
Medical Nutritional Therapy
Just as there is no single medical regimen that fits all patients, there are no ADA diets that can be prescribed. An individualized nutrition care program must be customized to each patient's specific preferences and needs based on a comprehensive assessment. Integrating insulin therapy with an individual's food and activity preferences is central in the management and education of patients with Type 1 diabetes. While many issues are identified during the assessment phase, glycemic control is usually addressed first, followed by nutritional interventions related to improvement of dyslipidemia and blood pressure.
As we discussed in the previous Cyberounds® on this case, the T1DM patient must learn how to manage hypoglycemia not only for immediate safety but also because over-treating and/or fear of hypoglycemia are frequent barriers to reaching long-term glycemic goals. Some patients overeat and administer inadequate insulin in order to avoid hypoglycemia. These are not desirable strategies. While recognition and treatment of hypoglycemia are relatively straightforward, hypoglycemia prevention often requires detailed records and patient-provider teamwork. Patients need to learn the fine balance between food, exercise and medications as it relates to glycemia.
An important component of self-management is blood glucose monitoring. Choices of blood glucose monitors are plentiful; all meters are fast, and accurate when used correctly. Choosing one is based on individual preference and insurance reimbursement. Demonstration is effective in assessing technique and building patient confidence. The toll-free 800 number on the back of each monitor is useful for trouble shooting. Frequency and timing of testing need to be individualized according to the type of insulin regimen and changes in therapy. For instance, a patient with Type 1 diabetes who requires four injections or more will need to monitor at least four to eight times daily, while a patient requiring basal insulin only may not need to check their blood sugar more often that once or twice daily. Target blood sugar ranges need to be reviewed to interpret insulin effects and determine therapeutic changes.
Carbohydrate Counting
Bolus dosing before meals requires the advanced skill of carbohydrate counting for the purpose of determining the correct pre-meal dosage of rapid-acting insulin. The carbohydrate content of food can be found on a food label, in carbohydrate counting books and apps, or by learning that fixed serving sizes for each carbohydrate food contains 15 grams of carbohydrate. For example, one small piece of fruit or half a large piece of fruit each contains 15 grams. Some studies, including the DAFNE program, examining type 1 diabetics have shown significant improvements in HbA1c once taught carbohydrate counting programs, although many do not have control groups. (46)
Carbohydrates are the main nutrients that impact blood sugar, more so than proteins or fats.(38) A large meal of bacon and eggs has minimal carbohydrate content and, therefore, significantly less effect on blood sugar. The established theory has been that blood sugar rise is much more related to the total amount of carbohydrate than the source of carbohydrate.(38) For example, two slices of bread and six Mini Tootsie Rolls have the same carbohydrate content and, therefore, raise blood sugar similarly. However, the body of research is growing indicating that glycemic index, and thus the type of carbohydrate, may also play a large role in the glucose peak and length of glucose excursion.(46) Glycemic control can be achieved regardless of the amount or type of carbohydrate ingested as long as adequate insulin is administered. The most common carbohydrate counting mistakes by patients are identifying carbohydrate sources incorrectly, estimating portions incorrectly, misreading labels and snacking without administering insulin.
As the patient's CIR is one unit rapid-acting insulin for every 10 grams of carbohydrate, 9 units are needed for the 90-gram breakfast. Since the patient needs to drop 40 mg/dl to reach the pre-meal target of 100 mg/dl, an additional unit is required since one unit drops his blood sugar by 40 mg/dl (CF = 40).
Nine units may result in hyperglycemia. As the patient's CIR is one unit rapid-acting insulin for every 10 grams of carbohydrate, nine units are needed for the 90-gram breakfast. Since the patient needs to drop 40 mg/dl to reach the pre-meal target of 100 mg/dl, an additional unit is required since 1 unit drops his blood sugar by 40 mg/dl (CF = 40).
Eleven units may cause the patient to go low. As the patient's CIR is one unit rapid-acting insulin for every 10 grams of carbohydrate, nine units are needed for the 90-gram breakfast. To correct for the high pre-meal blood sugar and reach the target of 100 mg/dl, an additional unit of insulin is needed to drop the sugar 40 m/dl (CF = 40).
Cream cheese contains minimal carbohydrate. Carbohydrate is the main nutrient that impacts blood sugar, not protein or fat.
Individuals vary considerably in the amount of insulin needed for a fixed amount of carbohydrate. A commonly used method for estimating a patient's individualized carbohydrate to insulin ratio (CIR), the amount of carbohydrate that one unit of rapid acting insulin will cover, is to divide 500 by the average number of total daily units of insulin (rapid and long-acting) administered each day.(*) A patient on an average of 30 units of insulin per day would have a CIR of about 15:1 (500 divided by 30 equals 16.6). In other words, one unit of rapid-acting insulin is needed for 15 grams of carbohydrate. Factors that affect insulin sensitivity can change an individual's CIR. For instance, exercise will improve insulin sensitivity. An individual with a CIR of 15:1 who anticipates eating two cups of rice (90 grams of carbohydrate) needs six units of rapid acting insulin. Once exercise is discontinued, the individual's sensitivity may decrease and the same two cups of rice would now require more insulin. A rise in blood sugar from a meal of more than 50 mg/dl may be a sign of either incorrect carbohydrate counting or an incorrect CIR. More recent research has shifted from looking solely at CIR to adjusting insulin based on the glycemic index rather than carbohydrates alone. (46)
In addition to the insulin dose needed to cover the carbohydrate, a supplemental dose may be required to correct for a high pre-meal blood sugar. This dose is referred to as the correction factor (CF) or the amount that one unit of insulin can be expected to decrease the level of glucose. The CF can be estimated by dividing the total number of units of daily insulin into 1500.(39) For example, someone who requires a total daily insulin dose of 50 units can have their insulin sensitivity factor calculated by the following: 1500/TDD = 1500/50 amounts to 30 (one unit of insulin will drop the blood sugar by 30 mg/dl). An individual with a target pre-meal blood sugar of 100 mg/dl whose CF is 40 (one unit of rapid acting insulin drops the blood sugar 40 mg/dl) and whose pre-meal CBG is 180 mg/dl, needs an additional two units above and beyond the amount of insulin calculated to cover the anticipated amount of carbohydrate. For those individuals who find advanced carbohydrate counting too difficult, a fixed dose regimen (to a greater or lesser extent) can be provided. This, however, imposes the challenge of consistency in timing and carbohydrate content of meals.
Without detailed blood sugar, food, exercise and insulin-dosing records, it is difficult to identify problems and make appropriate therapeutic changes. A three-day record can provide enough of a glimpse into the complex but typically patterned lifestyle of each individual. To achieve successful treatment adherence, the health care provider must stress to their patient the importance of meaningful and engaged office visits. The rigor of intensive insulin therapy demands repeated visits by the patient and negotiations among team members. Good practice for intensive insulin therapy also requires multiple visits to a registered dietitian, preferably a CDE, during the first three months totaling three to four hours, as well as four to six additional hours of follow-up during the year. Attention to dietary management of lipids, blood pressure and weight require additional visits.
The advantage of intensive insulin therapy using carbohydrate counting is the ability to achieve glycemic control without compromising flexibility in timing and content of meals. Glycemic control can be achieved even when skipping meals or eating more than usual. Of course, chronic overeating will result in weight gain. Patients learn to adjust their rapid acting insulin doses before meals according to the amount of carbohydrate they eat. Often, patients who carbohydrate count need to be reminded that high blood sugars from a meal are not from "too much" carbohydrate but rather arise as a result of inadequate insulin.
The advantage of intensive insulin therapy using carbohydrate counting is the ability to achieve glycemic control without compromising flexibility in timing or content of meals. Patients on fixed dose regimens of rapid acting insulins need to eat fixed amounts of carbohydrate; this regimen is seldom kept by the majority for prolonged periods of time, affects quality of life and rarely achieves optimal glycemic control.
It is the total amount of carbohydrate and not the source that impacts on blood sugars. As long as one counts carbohydrates and takes the corresponding amount of insulin to match the carbohydrate, glycemic control can be achieved. In practice, drinking large amounts of sugary beverages can be hard to manage due to the high caloric intake.
The advantage of intensive insulin therapy using carbohydrate counting is the ability to achieve glycemic control without compromising flexibility in timing or content of meals. On the other hand, patients on fixed combinations need to eat fixed amounts of carbohydrate at regular times in order to match the peaks of the insulins injected.
Glycemic index of foods does not impact as much on blood sugars as the total amount of carbohydrate.
Case Report Laboratory data showed that the HbA1c improved from 11% to 7.2%. The patient returned to the nurse to review glucose records and to discuss the need for regimen changes. His records showed elevated fasting and nocturnal glucose levels. After a team discussion, it was decided to perform a 72-hour continuous glucose monitoring sensor test to better identify glucose trends and make more effective therapeutic choices. The team strongly reminded the patient that tight glycemic control (an HbA1c close to 6%) is paramount if the patient wants to avoid micro and macrovascular complications. |
Continuous Glucose Monitoring Sensor (CGMS)
CGMS is used when more intensive monitoring is required. These systems are usually comprised of a sensor, a transmitter and a receiver.(47) A glucose sensor, placed under the abdominal skin, measures interstitial glucose every 10 seconds and these glucose values are averaged every five minutes. These measurements are highly correlated with finger stick values.(40) The information from the sensor is sent to the transmitter which is connected to the sensor but sits on the skin. The information is relayed from transmitter wirelessly to the receiver which can be a dedicated device, smart phone, or insulin pump.(47)
The results can be read in real time, on demand or downloaded to a computer where graphs and tables reveal glucose trends. These devices can be especially helpful in complicated situations such as hypoglycemia unawareness, gastroparesis, gestational diabetes, preconception, pregnancy and lactation where the patient and doctor want to achieve tighter control. By obtaining frequent glucose values, individuals can more readily see the effect of diet, exercise and medications in order to make the needed changes that will result in fewer glucose excursions.
Recent analyses have shown patients with Type 1 Diabetes reaching a lower A1c when using real time CGM vs. intermittent self-monitored blood glucose without significant increases in hypoglycemia.(14)(47) Evaluation of the JDRF-CGM Study Group also showed significant reductions in A1c with CGM and significant reductions in hypoglycemia.(48) A recent study in Sweden similarly showed significant improvements in A1c with CGM compared to conventional therapy, and additionally improved well-being in the CGM group.(49) The American Association of Clinical Endocrinologists and American College of Endocrinology recently released a consensus statement regarding CGM stating: "CGM improves glycemic control, reduces hypoglycemia, and may reduce overall costs of diabetes management. Therefore, expanding CGM coverage and use would improve the health of the diabetes population."(50)
The mean blood glucose concentration obtained postprandially (one to two hours after a meal) primarily reflects the effectiveness of the bolus insulin dose. Postprandial values indicate if adequate bolus insulin was given to match the amount of carbohydrate consumed.
The mean blood glucose concentration before meals (before breakfast, before lunch and before dinner) primarily reflects the effectiveness of the basal insulin.
A nocturnal test reflects the effectiveness of the basal insulin overnight. It is common to see a sharp rise in blood glucose beginning at 2:00AM-3:00 AM from the dawn phenomenon.
The fasting blood glucose level reflects the adequacy of the overnight basal insulin.
The blood glucose level post exercise may reflect either basal or bolus excess, depending upon when the exercise took place. Generally, if the activity takes place within three hours after eating, a 50% reduction of mealtime insulin should be recommended. If the exercise takes place before the meal or lasts longer than 30 minutes, a reduction in basal insulin for 24-48 hours may be necessary, as glucose levels may be affected up to 48 hours later. To prevent hypoglycemia, extra carbohydrate calories may also be necessary prior to exercising.
Case Report, Continued Three days later, the sensor was downloaded and showed consistent elevated glucose levels between 3:00AM and mid-morning. Two possible regimen changes were discussed:
The patient elected to continue multiple daily injections. In an attempt to further improve his glycemic control, he asked about adding pramlintide to his current regimen. It was explained that although pramlintide improved hyperglycemia, it was not realistic at this time, as it would mean at least eight injections daily. The team promised to evaluate pramlintide in the future once a repeat A1C is obtained and/or if the patient decides to change to the insulin pump (continuous subcutaneous insulin infusion). |
Continuous Subcutaneous Insulin Infusion (CSII)
Continuous subcutaneous insulin infusion (CSII) a method of delivering insulin through a motor driven reservoir into a self-inserted subcutaneous infusion set; the insulin serves as both basal and bolus. All rapid-acting insulin analogues are more effective than regular insulin in insulin pumps — they achieve better glycemic reductions in postprandial blood glucose concentrations and provoke fewer episodes of hypoglycemia compared with regular insulin.(41)(42) The basal insulin consists typically of 40-60% of the total daily dose and is individually programmed and adjusted by 0.05 units every 30 minutes to match the changes in basal needs throughout the 24-hour day. Insulin delivered via CSII is absorbed better and more predictably than the "depot" of insulin delivered in multiple daily injections (MDI).(14)
The pre-meal bolus insulin amount can be automatically calculated by programming the pump for the patient with pertinent figures including the carbohydrate to insulin ratio, correction factor, glycemic targets and duration of insulin action. The patient enters the anticipated carbohydrate amount and blood sugar. The calculation takes into account the active insulin on board, subtracting this insulin from the estimated correction dose, thereby avoiding stacking of insulin and hypoglycemia. Pump features that promote individualization include bolus delivery over an extended period to match prolonged digestion and absorption of food. For example, a high fat meal treated with an injection of rapid-acting insulin often results in an initial hypoglycemic response followed by hyperglycemia when the food finally is finally absorbed.
Some studies comparing MDI to CSII demonstrate comparable HbA1C values, though patients on CSII report less hypoglycemia, post-meal glucose excursions and better quality of life.(42) Although a meta-analyses looking at analogue CSII alone vs MDI found no difference in hypoglycemia levels in adults with Type 1 Diabetes.(51) Some disadvantages of the insulin pump are the higher cost for the pump and its supplies, increased skin infections at the insertion site and greater chance of mechanical problems such as interruption of insulin flow or pump failure that can lead to diabetic ketoacidosis (DKA). An early malfunction that is not recognized can lead to DKA within four to six hours. Therefore, it is imperative for all individuals using an insulin pump to test blood glucose levels frequently (no less then four to six times each day), be properly trained in the use of the pump and learn how to avoid and treat acute complications proactively. It is important that those who choose the pump as a delivery system clearly understand that the convenience of no injections is offset by many other responsibilities and that the pump is a delivery system that is only as effective as its user.

Figure 3. Illustration of Two Insulin Pumps.

Continuous Subcutaneous Insulin Infusion (CSII) - most recent development of the closed loop system
Size - 3.8" x 2.0" x 1.00"
Weight - 3.7 oz (with battery)

In September 2016 the FDA approved the first hybrid closed-loop system to automatically monitor and deliver insulin.(52) These systems provide a basic background amount of insulin based on feedback from glucose readings, while the patient still controls the pre-meal boluses. Studies with hybrid closed-loop systems show an increase in the time spent in in the glucose target range and a reduction in the time spent in the hypoglycemic range.(48)
Summary
This is a case of a 51-year-old male who developed Type 1 diabetes also known as Latent Autoimmune Diabetes of the Adult (LADA). In the first Cyberounds® on this case, we reviewed how to establish a correct diagnosis, the essentials of patient education and the importance of early and aggressive treatment. Here, we have discussed intensive insulin management using a team approach. The prescription of an effective basal-bolus regimen is intricate and requires a team effort that includes the patient, nurse, dietitian, endocrinologist and others. This labor-intensive endeavor needs to be individualized through trial and error. A variety of insulins including the more recent analogues enable better physiologic insulin replacement treatment, with the majority of patients being treated with a basal-bolus regimen. Proper adjustments of bolus insulin need to be done according to carbohydrate counting and the constant variations in insulin sensitivity.
In addition to traditional injectable insulin, the FDA has approved an injectable non-insulin amylin analogue and a non-injectable inhaled insulin. The wide choice of new medications and gadgetry include pen syringes, insulin pumps and better systems for monitoring, all of which have made management of Type 1 diabetes easier. These advances have improved insulin administration and adherence, reduced episodes of hypoglycemia and fostered a better quality of life for patients but they have only had a modest impact on glycemic control. The Continuous Glucose Monitoring Sensor (CGMS) has slowly evolved into a closed loop system where glucose sensors will provide feedback to implantable insulin pumps so as to deliver insulin requirements more precisely. It must always be remembered, however, that successful outcomes can only be achieved when effective team management and education are provided in combination with a patient who is proactively involved in self-management.