Course Authors
Frank A. Laws, M.D., and Richard W. Smalling, M.D., Ph.D.
Release Date: 12/26/2001
Upon completion of this Cyberounds®, you should be able to:
Identity which parameter of blood pressure yields the best prognostic information in hypertensive patients at risk for cardiovascular disease
Identify the blood pressure profiles that represent the best therapeutic goals in hypertensive patients who are at risk for the development of cardiovascular disease
Discuss why evaluation of other indices of arterial load and stiffness can lead to the early identification and treatment of patients at risk for the development of cardiovascular disease.
This Cyberounds® Cardiovascular Medicine puts forward a slightly new perspective on the treatment of hypertension, particularly in those who are at risk for cardiovascular events. Aggressive control of blood pressure has recently been shown to be very desirable in view of the decrease in events seen in patients with lower blood pressure target levels. Dr. Laws will review the particular relevance of arterial wall compliance as a possible risk factor in addition to the absolute levels of diastolic and systolic blood pressure. Please welcome Dr. Frank Laws back to Cyberounds®!
-- Richard W. Smalling, M.D., Ph.D., Cardiovascular Moderator
Arterial hypertension, defined as a systolic blood pressure (SBP) in excess of 140 mm Hg and/or diastolic blood pressure (DBP) in excess of 90 mm Hg, has long been identified as an independent risk factor for cardiovascular disease. Traditionally, emphasis has been placed on elevated DBP as a risk factor for the development of target organ damage. However, as early as 1971, the Framingham study showed that, although DBP was a major determinant of cardiovascular risk in men under 45 years of age, SBP was the stronger risk factor in older men and in women of all ages.(1) Since then, several observational studies have suggested that the pulse pressure (PP) may be a better predictor of cardiovascular complications than SBP or mean arterial pressure.(2),(3),(4),(5),(6)
Data from the National Health and Nutrition Examination Survey has demonstrated that if a blood pressure (BP) of 140/90 mm Hg is considered to be normal, only 27% of hypertensive patients are adequately controlled in the United States. Recommendations from the Joint National Committee on the Prevention, Detection, Evaluation and treatment of High Blood Pressure (JNC-VI report) now regard a BP of 140/90 mm Hg as high normal and 130/85 mm Hg as normal.(7),(8) For diabetic patients, therefore, it is recommended that BP be reduced below 130/85 mm Hg and for those with renal impairment, evidenced by proteinuria, pressures should be reduced below 125/75 mm Hg. In patients with underlying coronary artery disease, the BP should be reduced below 120/80 mm Hg.(9),(10)
The beating heart generates pressure and flow waves which propagate throughout the arterial system. The shape of the pressure and flow waves is altered by their continuous interaction with the non-uniform arterial system. The pressure and flow waves can be studied in terms of a forward component, running from the heart itself, and a backward component carrying information on the peripheral arterial system.(11)
In the presence of arteriosclerosis and aortic stiffening (consequences of arterial hypertension), the pulse wave velocity is increased, causing the pulse waves to reflect more quickly off the arteriolar vessels and return to the large vessels during systole. This amplifies SBP. In the presence of normal vascular compliance, the reflected waves return during diastole and augment DBP. Consequently, arteriosclerosis tends simultaneously to increase SBP and decrease DBP, resulting in a widened pulse pressure.
A widened pulse pressure increases cardiovascular morbidity because elevated SBP is associated with greater left ventricular workload and myocardial oxygen demand, whereas a decreased DBP may decrease coronary perfusion, resulting in decreased myocardial oxygen supply and a greater risk for myocardial ischemia and injury.(12)
In this Cyberounds®, we will review the basic pathophysiologic mechanisms underlying the cardiovascular complications of arterial hypertension. Other indices of arterial hypertension that reflect arterial stiffness will be discussed and the clinical evidence supporting the usage of these indices in clinical practice will be reviewed. Finally, current management options and future directions will be outlined.
Cardiovascular Complications of Hypertension
The involvement of the renin-angiotensin-aldosterone system (RAAS) and the endothelin system in the development and maintenance of arterial hypertension leads to the activation of signal transduction pathways which have deleterious effects at the cellular level of the myocardium. Angiotensin II and endothelin I, end products of both systems, are potent vasoconstrictors which mediate myocyte hypertrophy and increased collagen synthesis and deposition.(13)
All forms of cardiac dysfunction are preceded by myocyte hypertrophy.(14) The development of reactive fibrosis, a consequence of increased collagen deposition, leads to impaired cardiac relaxation and, hence, diastolic dysfunction. As left ventricular hypertrophy (the result of myocyte hypertrophy and reactive fibrosis) develops, a myocardial oxygen demand-supply mismatch occurs leading to myocardial ischemia. The development of artherosclerosis, also a result of arterial hypertension and other known risk factors, further accentuates this mismatch by leading to endothelial dysfunction and later occlusive coronary disease (Figure 1).

Figure 1. The Interaction of the Angiotensin and Endothelin Systems Leading to Hypertension and Cardiac Dysfunction.
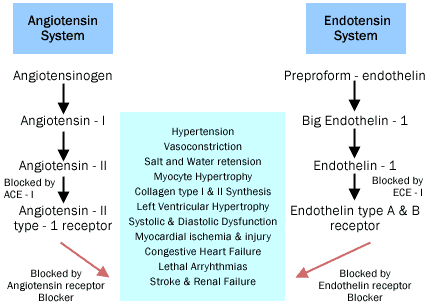

The development of left ventricular hypertrophy and myocardial ischemia both lead to impaired diastolic and systolic function. This later manifests as congestive heart failure, myocardial infarctions and lethal ventricular arrhythmias. Apart from effecting the myocardium itself, arterial hypertension also effects the vasculature of the kidneys and the brain adversely. Elevated SBP has been demonstrated as an independent risk factor for strokes and a reduction in SBP leads to a decrease in the incidence of strokes.(15) Reductions in mean arterial pressure and SBP also decrease the incidence of albuminuria and renal failure secondary to uncontrolled hypertension.(16)
Medical therapy with angiotensin converting enzyme inhibitors (ACEIs), angiotensin receptor blockers (ARBs) and calcium channel blockers (CCB) has been shown to lead to a reversal of LVH, a decrease in mortality associated with congestive heart failure, as well as a decrease in albuminuria and the rate of decline in renal function in patients with arterial hypertension.(17),(18) According to the JNC VI report, beta blockers and diuretics have been shown to be effective first line agents in the management of uncomplicated hypertension. Beta blockers are especially indicated in the management of patients with underlying coronary artery disease, as they decrease myocardial oxygen consumption and cardiac work, resulting in a decrease in cardiac mortality.
Indices of Arterial Load and Arterial Stiffness
Pulse Pressure (PP)
Blood pressure propagates through the arterial system as a repetitive continuous wave which consists of a pulsatile component (pulse pressure) and a steady component (mean pressure). The pulsatile component depends on left ventricular ejection, arterial stiffness and the timing of wave reflections, whereas cardiac output and vascular resistance determine the mean pressure. The pulse pressure (PP), measured as the difference between SBP and DBP at the brachial artery (PP = SBP - DBP); (PP = Ps - Pd; Figure 2), results at least partly from arterial stiffening. Arterial stiffening increases PP and backward reflections in the arterial system, leading to an increase in pulse wave velocity (PWV) and an augmentation of systolic pressure.(1)

Figure 2. A Central Aortic Pressure Wave Form.
Augmentation index (AIx) = (DP/PP) x 100
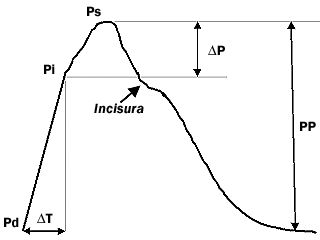
Pd: Diastolic Pressure
Pi: Inflection Pressure
Ps: Systolic Pressure
PP: Pulse Pressure

Pulse Wave Velocity (PWV)
Arterial stiffness can be assessed noninvasively in large populations by measurement of PWV. PWV is measured along the descending thoracoabdominal aorta. Pulse waveforms are obtained transcutaneously over the common carotid artery and the right femoral artery and the time delay (t) is measured between the feet of the two waveforms. The distance (D) covered by the waves is equilibrated to the distance measured between the two recording sites. PWV is calculated as [PWV = D (meters)/t (seconds)]. In a group of 418 subjects, Roland Asmar et al. showed with multiple regression analysis that pulse wave velocity correlated positively and independently with age and SBP by the equation PWV = 0.07 x SBP (mm Hg) + 0.09 x Age (y) - 4.3 (m/s) [meters/second].(19),(20)
Aortic Augmentation Index (AIx)
Augmentation index (AIx) is a measure of systemic arterial stiffness derived from the ascending aortic pressure waveform. The measured aortic pressure consists of incident and reflected waves, their magnitude and timing determine the aortic wave contour. In the young, the reflected waves arrive in the ascending aorta in late systole and generate the typical type-C pressure wave. In the presence of hypertension, the magnitude and speed of the reflected waves increase and they add to the forward wave in early systole, boosting systolic pressure and generating the typical type-A aortic pressure profile (Figure 3).

Figure 3. Type A and Type C Central Aortic Pressure Waveforms
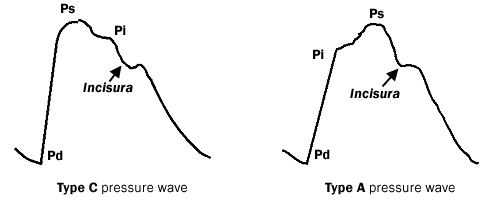
Click to see full sized image
Pd: Diastolic Pressure
Ps: Systolic Pressure
Pi: Inflection Pressure

The AIx is defined as the increment in pressure from the first shoulder (inflection point) to the peak pressure of the aortic pressure waveform expressed as a percentage of the peak pressure, [AIx (%) = (Ps - Pi) x 100/(Ps - Pd)], where Pi represents the inflection pressure as seen in Figure 2.(21),(22)
Other Indices of Arterial Load
Effective arterial elastance (Ea), which is the ratio between aortic end-systolic pressure and stroke volume, was first introduced by Sungawa et al. as an estimate of arterial load. Because it integrates peripheral resistance, total vascular compliance, characteristic impedance, as well as systolic and diastolic time intervals, Ea is considered a useful parameter under conditions such as aging and hypertension.(23),(24)
Another estimate of arterial compliance is the stroke volume-to-pulse pressure index, [C = (SV)/PP]. This index measures the ability of the arterial system to accommodate further increases in volume. Although both of these indices are obtained by invasive assessment of stroke volume, they can also be obtained by echocardiographic analysis of the aortic valve area and Doppler flow.(25)
Clinical Evidence
From a meta-analysis of three trials concerning systolic hypertension in the elderly: the European Working Party on High Blood Pressure in the Elderly trial, the Systolic Hypertension in Europe Trial (Syst-Eur) and the Systolic Hypertension in China Trial, Blacher et al. reported that a 10 mm Hg increase in pulse pressure increased the risk of cardiovascular mortality by nearly 20%.(2)
In the Boston Veteran's Administration Study of healthy male volunteers aged 21 to 80 years at enrollment, cardiovascular death was related to baseline SBP in younger (<60 years) subjects, while in older (>60 years) subjects PP appeared to be a more accurate predictor of death than SBP or DBP.(4) In a study of >19,000 men initially aged 40 to 69 years, brachial PP was a predictor of cardiovascular mortality over a mean follow-up of 19.5 years.(5) This association was evident at both low and high mean pressure. In the Studies of Left Ventricular Dysfunction (SOLVD), patients with impaired LV function, in which more than 70% had a previous myocardial infarction, baseline brachial PP was a predictor of total and cardiovascular mortality. Brachial PP remained a predictor in multivariate analysis even after adjustments for mean pressure and a range of other covariates.(6)
In a cohort of 1980 essential hypertensive patients where aortic stiffness was assessed by carotid-femoral PWV, multivariate models of logistic regression analysis revealed that PWV was significantly associated with all-cause and cardiovascular mortality, independent of previous cardiovascular diseases, age, and diabetes.(26) In the Pulse Wave Velocity as an endpoint in large-scale intervention trial (The Complior ® study), the feasibility of a large-scale intervention trial, using carotid-femoral PWV as the endpoint in hypertensive patients, was demonstrated.(27)
Therapeutic Targets
Despite the impressive epidemiological associations between PP and cardiovascular end points and outcomes, more evidence is required before it can be concluded that a reduction of PP should be a therapeutic goal. However, as the focus of attention in preventing and treating cardiovascular disease is shifting towards the arterial wall, the assessment of parameters that better evaluate arterial compliance will become more important.(28) The recently published Complior® study reflects a move in this direction.(27)
Several randomized studies have demonstrated the efficacy of ACE inhibitors to decrease PWV in hypertensive patients. In one study, drug therapy was able to reduce PWV within 42 days. In a double blind, crossover comparison trial, CCBs were shown to effect a more pronounced fall in PWV compared to diuretics.(29),(30)
The targeting of elevated SBP to achieve optimal blood pressure control (<130 mm Hg) will lead to a reduction in PP and other parameters of arterial compliance. A number of studies have suggested that ACE inhibitors and to a lesser extent calcium channel blockers exert direct arterial wall effects and induce changes not only because of the passive effects of blood pressure lowering. A recent report demonstrated that quinapril, an ACE inhibitor with high affinity for tissue ACE, improved endothelial dysfunction in patients with systemic hypertension, whereas nitrendipine (CCB) did not, even though both drugs reduced BP to the same extent.(31)
Because of the need for more aggressive BP control in high-risk patients who are unlikely to reach target BP goals with monotherapy, it may be necessary to use combination therapy. Low-dose combinations of antihypertensive agents, such as an ACE inhibitor and a CCB, can provide additional control of hypertension, while minimizing the likelihood of dose-dependent adverse effects.(10) The combination of amlodipine 5 mg/benazpril 10 mg was shown to be superior to either drug alone, or placebo, in the reduction of sitting diastolic blood pressure in patients with essential hypertension.(32)
It is no longer sufficient to identify and manage hypertension by simply initiating treatment once an arbitrary level of BP has been reached. Therapeutic decision-making should use models that provide information about early arterial wall changes even before there is clinical evidence of an elevated blood pressure. This approach allows for the early risk stratification of patients and the use of agents that have been shown to have a positive therapeutic effect on the arterial wall.(28)